Diabetic Retinopathy
Learn about diabetic retinopathy, including symptoms, stages, diagnosis, and treatment options to help protect vision in people with diabetes.
- Home
- Diabetic Retinopathy
Overview
Diabetic retinopathy is a diabetes-related eye condition that damages the tiny blood vessels of the retina, the light-sensitive tissue at the back of the eye. It can affect people with either type 1 or type 2 diabetes, and the risk usually increases the longer you have diabetes and the less controlled your blood sugar is over time. One of the most important things to know is that diabetic retinopathy may not cause noticeable symptoms in the early stages. If it is not found and treated when needed, it can lead to serious vision loss. Regular dilated eye exams are an important part of protecting your sight if you have diabetes.
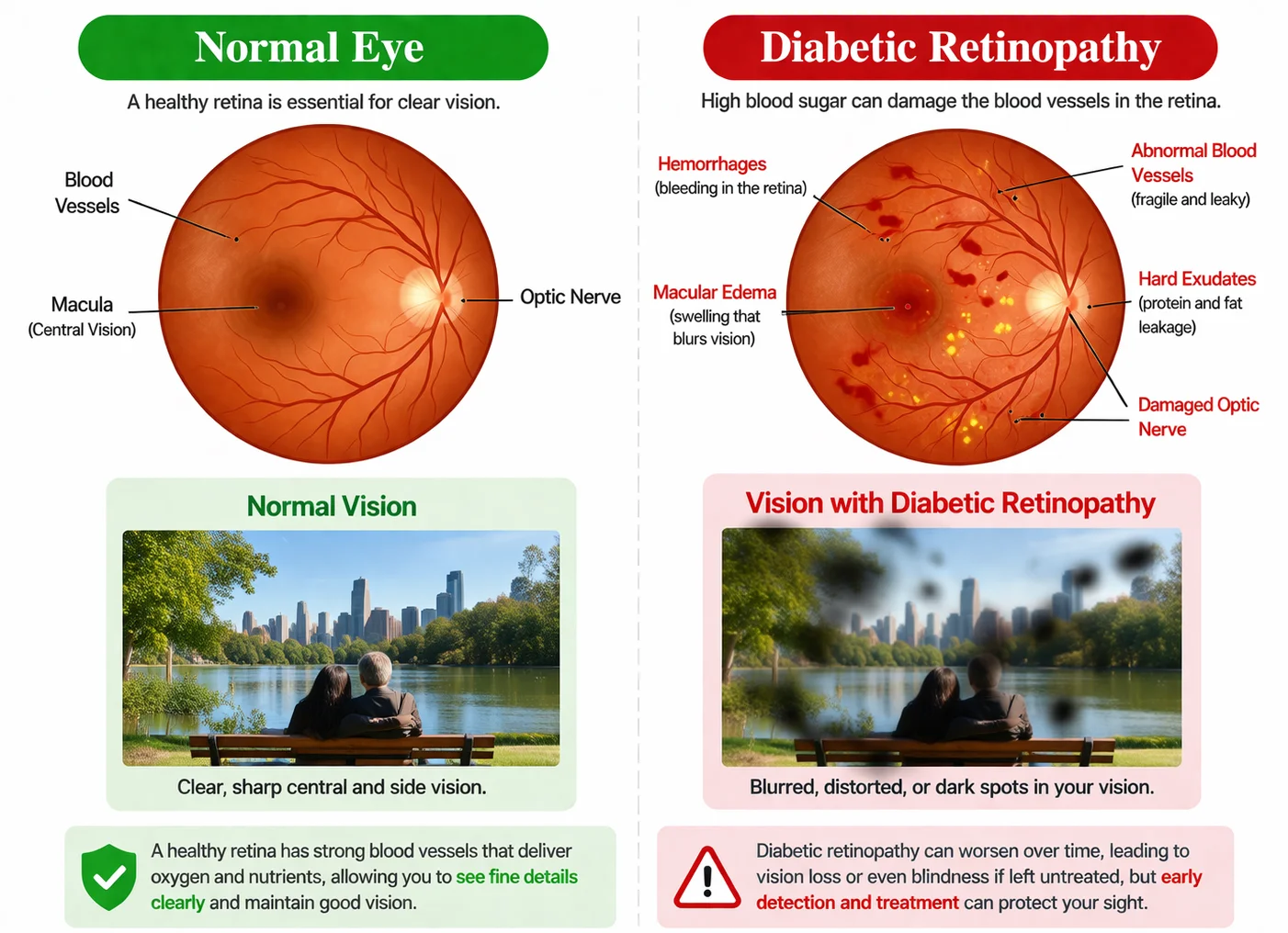
Learn more about Diabetic Retinopathy
Do I have Diabetic Retinopathy ?
Diabetic retinopathy often has no symptoms at first, which is why regular dilated eye exams are so important.
Symptoms of Diabetic Retinopathy
Symptoms can include, but are not limited to:
Spots or floaters
You may notice dark strings, spots, or drifting shapes in your vision.
Blurred or fluctuating vision
Vision may become blurry, inconsistent, or more difficult to keep in focus.
Dark areas or vision loss
Some people develop missing areas in their vision or more serious overall vision loss as the condition progresses.
Treatment of Diabetic Retinopathy
Treatment can range from monitoring to in-office or surgical care depending on severity:
Frequent dilated eye exams
Early diabetic retinopathy may simply be monitored closely so your doctor can track any changes in the retina.
Laser or injections
Laser treatment and medicine injections may help reduce leaking, swelling, or abnormal blood vessel growth.
Vitrectomy surgery
If there is a lot of bleeding or scar tissue in the eye, surgery may be recommended.

Whether you need a routine eye exam, upadet glasses or contacts, or help with an eye concert, our fiendly team is here to make the process easy.
- Personalized Care
- States-f-the-Art Equipment
- Experienced Optometrists
- Family-Friendly Environment

What causes Diabetic Retinopathy?
Diabetic retinopathy is caused by high blood sugar related to diabetes. Over time, too much sugar in the bloodstream can damage the tiny blood vessels that nourish the retina. These vessels may begin to leak, bleed, or close off. In response, the eye may try to grow new blood vessels, but these abnormal vessels do not work well and may leak or bleed easily. This damage can affect the retina itself and may lead to swelling, scar tissue, and progressive vision problems if not managed appropriately.
Getting a Diagnosis of Diabetic Retinopathy
Diabetic retinopathy is typically diagnosed during a comprehensive dilated eye exam. Because early disease may not cause symptoms, routine screening is one of the best ways to catch changes before they threaten vision.
Common tests used to diagnose diabetic retinopathy include:
Dilated Eye Exam
Eye drops are used to widen the pupil so your doctor can examine the inside of the eye and look directly at the retina and its blood vessels.
Optical Coherence Tomography (OCT)
OCT creates detailed images of the retina and can help your doctor identify swelling or thickening that may be present.
Fluorescein Angiography
This test uses a special dye and photographs to show whether retinal blood vessels are leaking, blocked, or growing abnormally.
Different stages of Diabetic Retinopathy
Diabetic retinopathy is often described in two main stages. Knowing the stage helps guide how closely the retina should be monitored and when treatment may be needed.
- Non-proliferative diabetic retinopathy (NPDR) is the earlier and more common stage, when tiny blood vessels leak, swell, or close off and may lead to macular edema or blurry vision;
- Proliferative diabetic retinopathy (PDR) is the more advanced stage, when abnormal new blood vessels grow, bleed into the vitreous, and may lead to scar tissue, retinal detachment, or severe vision loss.
Factors Increasing Risk of Diabetic Retinopathy
Anyone with diabetes can develop diabetic retinopathy, but some factors increase the risk or make the condition more likely to worsen over time.
Common risk factors for diabetic retinopathy include:
- Having diabetes for a long time
- Poor control of blood sugar levels
- High blood pressure
- High cholesterol
- Pregnancy
- Tobacco use
Questions about Diabetic Retinopathy?
We’re here to help protect your vision if you have diabetes. Whether you need routine retinal screening, answers about new vision changes, or guidance on treatment options, our team is happy to help you take the next step toward preserving your sight.
Diabetic retinopathy is a diabetes-related complication that damages the tiny blood vessels in the retina. Over time, those vessels can leak, bleed, close off, or trigger the growth of abnormal new vessels that threaten vision.
No. In the early stages, diabetic retinopathy may not cause noticeable symptoms. As it progresses, people may develop floaters, blurred vision, fluctuating vision, dark areas in vision, or vision loss.
Treatment depends on the stage and may include close monitoring with frequent dilated exams, laser photocoagulation, medicine injections, or vitrectomy surgery if there is significant bleeding or scar tissue.
Regular dilated eye exams, good blood sugar control, attention to blood pressure, and early treatment when changes are found can help reduce the risk of severe vision loss. You should also contact your eye doctor promptly if your vision becomes suddenly blurry, spotty, or hazy.