Keratoconus
Learn about keratoconus, including symptoms, causes, diagnosis, and treatment options such as specialty contact lenses, corneal cross-linking, Intacs, and corneal transplant.
- Home
- Keratoconus
Overview
Keratoconus is a condition in which the cornea, the clear front surface of the eye, becomes thinner and gradually bulges outward into a cone-like shape. As the cornea changes shape, light no longer focuses evenly, which can cause blurry, distorted, and often progressively worsening vision. Keratoconus usually affects both eyes, although one eye is often worse than the other. It often begins during the teenage years or early adulthood and may progress slowly over time. In the early stages, vision may improve with glasses or contact lenses, while more advanced cases may need specialized treatment to help stabilize the cornea and improve visual quality.
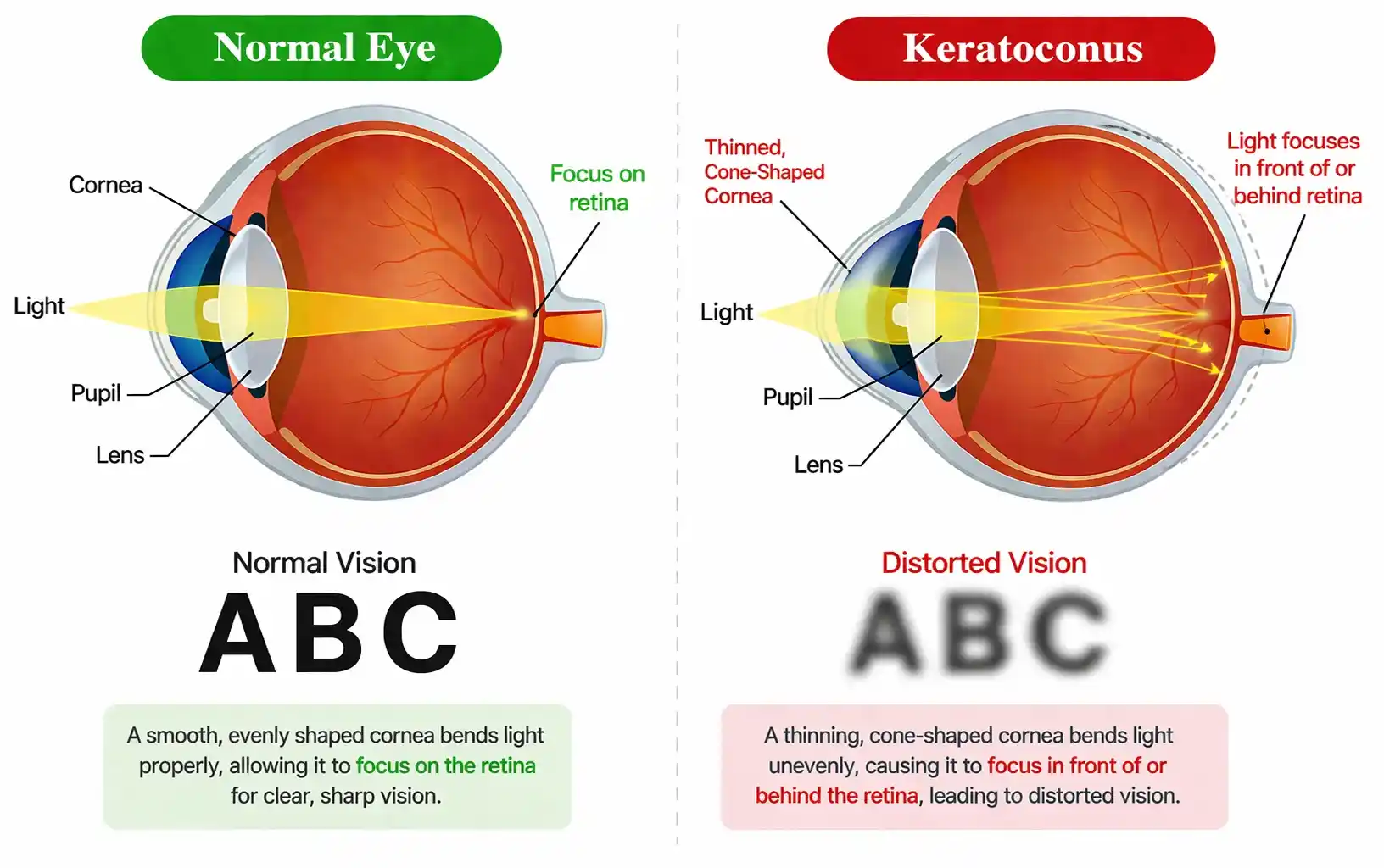
Learn more about Keratoconus
Do I have Keratoconus ?
Keratoconus often begins with subtle vision changes that become harder to correct as the cornea changes shape over time.
Symptoms of Keratoconus
Symptoms can include, but are not limited to:
Blurred or distorted vision
Vision may look smeared, doubled, or increasingly difficult to sharpen with glasses.
Glare, halos, and poor night vision
Lights may seem more glaring, especially at night, with halos or starbursts around them.
Light sensitivity, headaches, or frequent prescription changes
You may become more light sensitive and need updated glasses more often than expected.
Treatment of Keratoconus
Treatment depends on how advanced the condition is and how much the cornea has changed:
Glasses or soft contacts
These may help in mild cases, especially early on, though they often become less effective as keratoconus progresses.
Specialty contact lenses or cross-linking
Rigid gas permeable, hybrid, piggyback, or scleral lenses may improve vision, and cross-linking can help stabilize the cornea.
Intacs or corneal transplant
More advanced cases may need surgical treatment to improve shape or replace a scarred, severely affected cornea.

Whether you need a routine eye exam, upadet glasses or contacts, or help with an eye concert, our fiendly team is here to make the process easy.
- Personalized Care
- States-f-the-Art Equipment
- Experienced Optometrists
- Family-Friendly Environment

What causes Keratoconus?
Keratoconus develops when the cornea becomes weaker and thinner over time, allowing it to bulge outward into an irregular cone-like shape. The exact cause is not always clear, but genetics appear to play a role in some patients. Keratoconus is also associated with chronic eye rubbing, allergies or long-term eye irritation, and certain systemic disorders. Because the cornea becomes structurally weaker, the condition may continue to progress unless it is monitored and, when appropriate, treated to help stabilize it.
Getting a Diagnosis of Keratoconus
Keratoconus is diagnosed during a comprehensive eye exam, often with additional testing to measure the shape and thickness of the cornea. Early diagnosis is especially important because treatment may help slow or stabilize progression.
Common tests used to diagnose keratoconus include:
Corneal Topography
This is one of the most useful ways to detect keratoconus early. It creates a detailed map of the cornea’s curvature and shows whether the shape has become irregular.
Slit-Lamp Examination
A slit-lamp exam allows your doctor to closely inspect the outer and middle layers of the cornea for thinning or other changes.
Pachymetry
Pachymetry measures corneal thickness and can help identify thinning, including the thinnest areas of the cornea.
Stages and treatment of Keratoconus
Keratoconus often becomes more noticeable over time, and treatment choices usually depend on how much the cornea has changed and how well vision can still be corrected.
- Early keratoconus may be managed with glasses or soft contacts, although vision often becomes harder to sharpen as the cornea grows more irregular;
- Moderate keratoconus often benefits from specialty contact lenses such as RGP, piggyback, hybrid, or scleral lenses for clearer vision and better comfort;
- Progressive keratoconus may be treated with corneal cross-linking to strengthen the cornea and help slow further progression;
- Advanced keratoconus may require Intacs or a corneal transplant if the cornea becomes severely distorted or scarred.
Factors Increasing Risk of Keratoconus
Some people are more likely to develop keratoconus or see it progress more quickly than others.
Common risk factors for keratoconus include:
- Family history of keratoconus
- Certain systemic disorders, including Down syndrome
- Chronic eye inflammation from allergies or irritation
- Frequent or aggressive eye rubbing
- Teenage or young-adult onset
Questions about Keratoconus?
We’re here to help you understand keratoconus clearly and guide you toward the treatment that best fits the stage of your condition. Whether you need updated testing, clearer vision with specialty lenses, or treatment to stabilize the cornea, our team is happy to help you take the next step toward protecting your sight.
Keratoconus is a condition in which the cornea thins and gradually bulges outward into a cone shape. As that shape changes, light does not focus evenly and vision becomes more blurry and distorted.
Common symptoms include blurry vision, glare and halos around lights, poor night vision, light sensitivity, eye irritation, headaches, double vision, and frequent changes in glasses prescription.
No. LASIK is generally not recommended for people with keratoconus because it can weaken the cornea further and make vision worse. Your eye doctor can recommend safer treatment options based on the stage of your condition.
You should schedule an eye exam if your vision is worsening quickly, your prescription keeps changing, or you are having increasing glare, halos, or trouble seeing at night. Early diagnosis is important because some treatments can help slow progression.